


Pinpoint pupils are abnormally small, pinhead-sized pupils that barely react to light. They are one of the clearest signs that someone is suffering from an opioid overdose, which is why it’s important to know what drugs make your pupils small.
If you’ve ever found a loved one suddenly unresponsive or breathing slowly, the size of their pupils tells you a lot in the first few seconds. Here at Porch Light Health, we know how quickly that moment can turn life-threatening, and we support people across Colorado and New Mexico through medication-assisted treatment delivered through clinics, mobile sites, and telehealth.
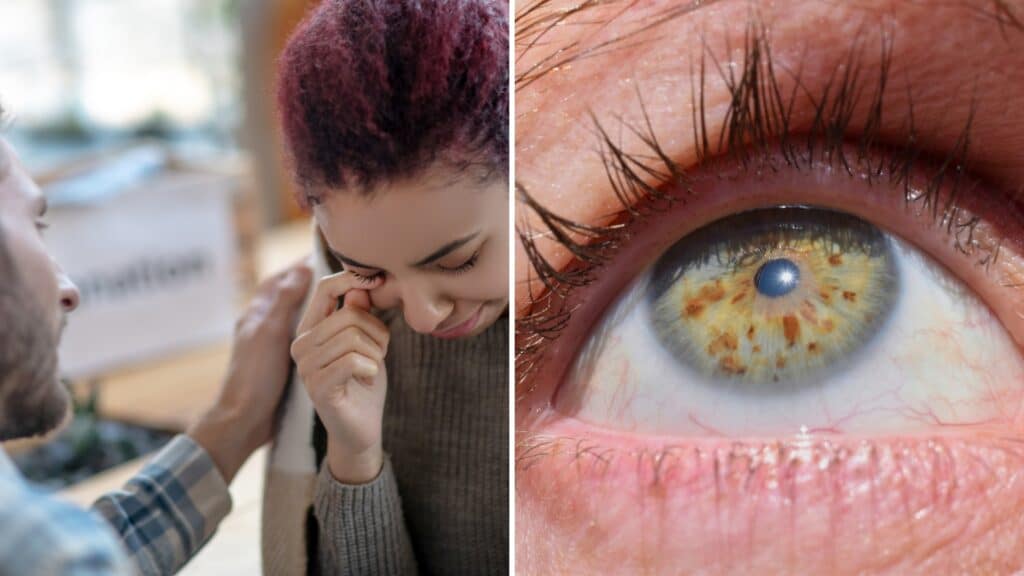
Pinpoint pupils, clinically called miosis, are pupils that are abnormally constricted. They’re caused by excess parasympathetic activity or reduced sympathetic tone, and they can reduce vision in dim conditions. At the bedside, pupil size is a quick visual cue for drug effects, toxin exposure, or focal neurologic injury.
Pinpoint pupils are a classic sign of opioid toxicity and can speed life-saving interventions like naloxone. Recognizing miosis alongside slow breathing and altered consciousness helps you prioritize emergency response and, when appropriate, immediate referral for opioid addiction treatment.
Recognizing which drugs constrict the pupil helps you identify possible opioid toxicity and get timely care. The most common drug classes that cause pinpoint pupils include:
Pinpoint pupils in an unconscious person raise suspicion for opioid overdose and justify giving naloxone when opioid toxicity is likely. Identifying the drug class also guides toxicology testing and urgent treatment decisions, because the right antidote depends on the cause.
For people whose pupils stay constricted from an active opioid use disorder, our Suboxone therapy and heroin addiction treatment programs help stabilize withdrawal and start recovery.
Opioids are the most common drug-related cause of miosis. Mu opioid receptor activation increases parasympathetic output to the iris, which produces the classic pinpoint pupil. A StatPearls clinical review of opioid toxicity describes the typical bedside triad of miosis, respiratory depression, and reduced consciousness.
Not every opioid exposure causes extreme pinpointing. Dose, the specific opioid, and any co-ingested substances all change how the pupil responds.
Central mu receptors increase parasympathetic tone to the iris sphincter, so pupil constriction often appears before breathing slows. This is part of why miosis is such a useful early warning sign in suspected overdose situations.
Clinicians watch for the triad of pinpoint pupils, respiratory depression, and decreased alertness. When these three signs appear together, it should be treated as a medical emergency until proven otherwise.
Both prescription opioids (morphine, oxycodone, hydrocodone, fentanyl patches) and illicit opioids (heroin, illicitly manufactured fentanyl) can produce miosis. Potency and formulation change how pronounced the effect is.
Co-ingestants like benzodiazepines may worsen respiratory depression even when pupils don’t look dramatically small. We support people affected by this through our fentanyl addiction treatment program, which includes harm-reduction conversations alongside MAT.
Non-opioid medications and toxins can also cause constricted pupils, and the cause shapes the treatment.
Organophosphate pesticides and nerve agents inhibit the enzyme acetylcholinesterase, which increases muscarinic stimulation of the iris sphincter and produces pinpoint pupils. Severe cases often need atropine, pralidoxime, decontamination, and rapid supportive care in a hospital setting.
Clonidine activates central alpha-2 receptors, shifting autonomic balance and causing miosis at therapeutic or overdose doses. Accidental ingestions in children and intentional overdoses are the most common scenarios where clonidine becomes clinically relevant, and they may need urgent monitoring.
Pilocarpine is a topical muscarinic agonist used intentionally in eye care to constrict pupils, especially during and after cataract surgery. Barbiturate-induced miosis is uncommon and usually appears only in deeply sedating overdoses. Benzodiazepines rarely cause miosis on their own but can show up alongside other agents in mixed exposures.
If you suspect a medication or exposure has affected someone you love, our outpatient withdrawal management services can help with safe stabilization close to home.
If small pupils are persistent and don’t have an obvious drug or toxin explanation, several medical and neurologic conditions are worth considering.
Horner’s syndrome typically presents as a unilateral small pupil with a drooping eyelid on the same side and reduced facial sweating. Because it can indicate carotid artery dissection or a lung apex tumor, it warrants urgent imaging and vascular evaluation.
Inflammation can cause a constricted pupil with eye pain, light sensitivity, and a red eye. Prompt treatment helps prevent posterior synechiae and lasting vision loss.
These pupils are small, irregular, and accommodate to near targets but don’t react to light. When this pattern appears, syphilis testing is appropriate.
Lesions in the pons can produce pinpoint, reactive pupils together with reduced consciousness and motor deficits. This presentation needs immediate emergency care and neuroimaging.
Surgical scarring or severe prior inflammation can tether the iris to the lens, causing persistent irregular miosis. A slit-lamp exam clarifies the diagnosis.
Older adults commonly develop bilateral, gradual pupil constriction that worsens low-light vision. Simple optical aids or an ophthalmology consult may help when it limits function.
Recognizing the pattern (unilateral versus bilateral, painful versus painless, isolated versus paired with neurologic signs) helps you prioritize urgent testing and referral.
At the bedside, clinicians check direct and consensual light reflexes, near response, pupil symmetry in bright and dim lighting, and the speed of reactivity to summarize how the pupil is functioning. The steps below are how a typical evaluation unfolds:
If findings are ambiguous, careful documentation, short-interval follow-up, and targeted testing usually resolve the cause. For ongoing addiction care once the acute episode is stabilized, our behavioral health services integrate counseling with medication-assisted treatment.
Onset and duration vary by drug, dose, and route. Intravenous heroin or fentanyl can produce miosis within minutes that lasts hours, while oral opioids often constrict pupils for several hours. Organophosphate exposure causes rapid, often sustained miosis until the cholinergic toxicity is treated.
| Substance / Class | Typical Onset | Typical Duration |
| Intravenous Heroin or Fentanyl | Within Minutes | Several Hours |
| Oral Opioids (Oxycodone, Hydrocodone) | 30–60 Minutes | 4–8 Hours |
| Methadone, Extended-Release Opioids | 1–3 Hours | Up to 24 Hours |
| Organophosphate Pesticides | Minutes | Hours to Days, Until Treated |
| Clonidine | 30–60 Minutes | Several Hours |
| Pilocarpine Eye Drops | 10–30 Minutes | 4–8 Hours |
Tolerance can blunt visible miosis in chronic opioid users, which makes the classic sign less reliable in that population. Stimulants like amphetamine or cocaine and anticholinergic drugs dilate pupils and can offset opioid-related constriction, complicating the bedside picture in mixed exposures. A clear evaluation always considers timing, reported substances, and possible co-ingestants.
If you find someone with pinpoint pupils, check responsiveness and breathing, then call emergency services. For suspected opioid overdose, give naloxone if it’s available and follow the device instructions. Stay with the person and monitor breathing, because opioids can depress respiration and re-narcotize after a single naloxone dose wears off.
After the immediate emergency, clinicians can determine whether methadone treatment, further toxicology workup, or another targeted treatment makes sense.
If small pupils appear together with breathing trouble, unresponsiveness, or severe confusion, call 911 right away. Slowed breathing and unconsciousness are the clearest emergency signs to act on.
For safety, we recommend treating any suspected opioid exposure as an emergency, because respiratory collapse can develop quickly. Once the immediate risk is managed, our telehealth services make follow-up evaluation accessible no matter where you live in our coverage area.
Intraoperative floppy iris syndrome (IFIS) is worth flagging for anyone preparing for cataract surgery. IFIS is linked to alpha-1 blockers, most notably tamsulosin, and can cause iris billowing and unwanted pupil constriction during the procedure.
If you’ve ever taken tamsulosin or a similar drug, tell your surgeon, even if you stopped years ago. The history changes how the surgical team prepares.
IFIS makes the iris flaccid and prone to prolapse, which raises the risk of lens damage and adds operative time. Sharing your full medication history during preoperative review lets your team anticipate pupil behavior and prepare the right tools.
Pilocarpine drops are the main therapeutic myotic used to induce miosis during and after cataract procedures, helping stabilize the anterior chamber and reduce iris prolapse.
Knowing your medication history lets surgeons plan specific measures, such as intracameral phenylephrine, mechanical iris devices like iris hooks, or adjusted technique, all of which can lower complication rates when small pupils are anticipated.
Pupil size is one of the fastest clues to which class of substance might be involved in an intoxication. The table below summarizes the most common patterns; it’s a rough guide for recognition, not a substitute for a clinical evaluation.
| Substance / Class | Pupil Size | Other Common Signs |
| Opioids | Bilateral Pinpoint | Respiratory Depression, Decreased Consciousness |
| Organophosphates / Cholinergics | Pinpoint | Salivation, Sweating, Bronchospasm |
| Benzodiazepines / Sedatives | Small to Normal | Sedation, Slurred Speech |
| Stimulants (Amphetamines, Cocaine) | Dilated | Agitation, Fast Heart Rate |
| Anticholinergics (Some Antihistamines) | Dilated | Dry Skin, Hyperthermia |
| Opiate Withdrawal | Dilated | Yawning, Runny Nose, Anxiety |
If you suspect an opioid overdose, act quickly and seek urgent medical attention.
Spotting small pupils at the bedside often changes what happens next. Recognizing drug-induced miosis prompts naloxone administration, calling EMS for respiratory depression, or fast referral to medication-assisted treatment and counseling. For a deeper read on what comes after recognition, our blog on opioid use disorder explains the prevalence, diagnosis, and treatment options that follow.
That last step is where ongoing care begins. We’ve designed our network so that the moment someone is stabilized, there’s a clear next step, whether that’s a same-day phone call, a virtual intake, or a visit to one of our mobile sites.
If you’re reading this because of someone you love, you’ve already taken the hardest step: paying attention. Recognizing the signs is the beginning of getting them connected to care.
Here at Porch Light Health, we offer medication-assisted treatment, counseling, and harm-reduction support through clinics, mobile sites, and telehealth across Colorado and New Mexico. Same-day intake and insurance verification are part of how we keep treatment within reach. Whatever format fits your situation, we can help you find it. Call (866) 260-5340 to speak with us now.
What drugs commonly cause pinpoint pupils (miosis)?
Opioids are the classic cause, but other classes also produce miosis: cholinergic agents and organophosphate pesticides, therapeutic myotics like pilocarpine, alpha-2 agonists like clonidine, and some older sedative or antipsychotic medications. Organophosphate exposures usually include systemic cholinergic signs (sweating, vomiting, salivation) along with very small pupils, and pilocarpine is used intentionally in eye care to constrict the pupil.
Are opioids the main cause of drug-induced pinpoint pupils?
Yes. Opioids are the most common drug cause and the classic clinical association.
Mu opioid receptor activation increases parasympathetic input to the iris, which produces constricted pupils. This pattern is frequently seen with opioid toxicity and overdose.
Which prescription painkillers or illicit opioids most frequently cause miosis?
Most opioid family members can cause marked miosis, including heroin, fentanyl, morphine, oxycodone, hydrocodone, methadone, and buprenorphine. Fentanyl and potent synthetic opioids often produce more pronounced and sustained pinpointing than lower-potency oral opioids, while long-acting agents like methadone can keep pupils constricted for many hours, depending on dose and route.
Do medications like clonidine, barbiturates, or pilocarpine cause pinpoint pupils?
Yes for clonidine and pilocarpine. Clonidine reduces sympathetic tone and can cause mild miosis, and pilocarpine is a cholinergic eye drop intentionally used to constrict the pupil. Barbiturates rarely cause isolated pinpoint pupils on their own; when present, miosis usually reflects broader central nervous system depression from a high-dose sedative toxicity.
Can poisoning (organophosphates or other toxins) cause constricted pupils?
Yes. Organophosphate pesticide or nerve agent poisoning produces cholinergic excess with very small pupils, salivation, diarrhea, bronchorrhea, and muscle weakness.
Occupational and accidental exposures can present rapidly after contact. Other cholinergic drugs and toxins that stimulate the parasympathetic system can have the same effect.
What medical conditions cause miosis besides drugs?
Non-drug causes include Horner’s syndrome (usually unilateral miosis with eyelid droop and sometimes decreased facial sweating), ocular inflammation like iritis (often painful, with photophobia), Argyll Robertson pupil from neurosyphilis, and lesions in the pons or other brainstem locations that affect pupillary control. Age-related physiologic miosis can also make pupils appear small without underlying pathology.
How is drug-induced miosis treated in emergency settings?
Treatment targets the underlying cause. Suspected opioid overdose calls for prompt naloxone and airway support, because respiratory depression is life-threatening.
Organophosphate poisoning is treated with atropine, pralidoxime, and decontamination. Supportive care and monitoring are standard for sedative or mixed-toxicity cases.
When should I call 911 for someone with small pupils?
Call 911 immediately if the person is unresponsive, breathing slowly or not at all, is difficult to rouse, or shows signs of severe poisoning such as seizures, severe vomiting, or chest pain.
If the only finding is mild isolated miosis but you’re worried about recent drug use, seek urgent evaluation rather than waiting. Small pupils can signal a life-threatening overdose when paired with respiratory or mental-status changes.
Can benzodiazepines cause pinpoint pupils on their own?
No. Benzodiazepines typically cause drowsiness and slowed breathing at high doses but don’t reliably produce pinpoint pupils on their own. When miosis is present alongside benzodiazepine exposure, it usually reflects co-ingestion of opioids or another miosis-producing drug rather than the benzodiazepine itself.
How long do pupil-constricting effects usually last for different drugs?
Duration varies by drug and route. Intravenous fentanyl or heroin can produce noticeable miosis within minutes that lasts several hours. Oral short-acting oxycodone or hydrocodone typically causes effects for 4 to 8 hours.
Methadone and extended-release opioids can produce constriction for many hours, depending on dose. Organophosphate effects appear rapidly and persist until treated with antidotes and decontamination.
Individual tolerance, metabolism, and polysubstance use change these timelines. Clinical monitoring, rather than assumed timing, should guide care.
If you or someone you know may be at risk of opioid overdose or needs medication-assisted treatment, we can help. Here at Porch Light Health, we connect people across Colorado and New Mexico to clinics, mobile sites, and telehealth options for urgent assessment and ongoing MAT.
Reach out so a clinical team can help guide next steps and reduce immediate risks. Visit our Get Help Now page to start or call us at (866) 260-5340.
If you or someone you love is in crisis, you can also call or text 988 for the Suicide and Crisis Lifeline.






